All photography by Paul Fetters
At the Church of Scotland Hospital in Tugela Ferry, more than 460 patients have been diagnosed with drug-resistant TB since an initial outbreak there in February 2005. Overcrowded and poorly ventilated waiting areas full of HIV-infected patients with weak immune systems contribute to the spread of TB in KwaZulu-Natal province.


Living in rural areas, patients like B. Mazibuko of Tugela Ferry and N. Bgcob of Edendale have a hard time maintaining the grueling TB treatment regimen, which involves six months of daily injections followed by 12 to 24 months of pills. Only about 40 percent of patients in KwaZulu-Natal live to complete treatment.

Community is vital in rural KwaZulu-Natal province, where subsistence living is the norm. Health care workers join with tribal leaders and traditional healers to introduce Western medical treatments and promote education about HIV/AIDS and TB. More than 200 HIV-positive babies are born every day.

At the Prince Cyril Zulu Communicable Disease Center in the bustling port city of Durban, patients who typically come in complaining of a persistent cough leave with a diagnosis of both TB and HIV. The center, known to locals as the Durban Chest Clinic, will be linked to K-RITH.

To lend support and help ensure treatment compliance, health care workers at the Durban Chest Clinic ask patients with TB to return weekly for progress reports and to pick up their supply of medications. Completing the regimen is essential to curing the disease and stopping its spread.

Even at private facilities such as Durban’s McCord Hospital, founded by missionaries a century ago, research operations lack adequate resources. According to administrators, the biggest challenges are a lack of space, money, and trained researchers as well as meeting the psychosocial needs of patients and the community.
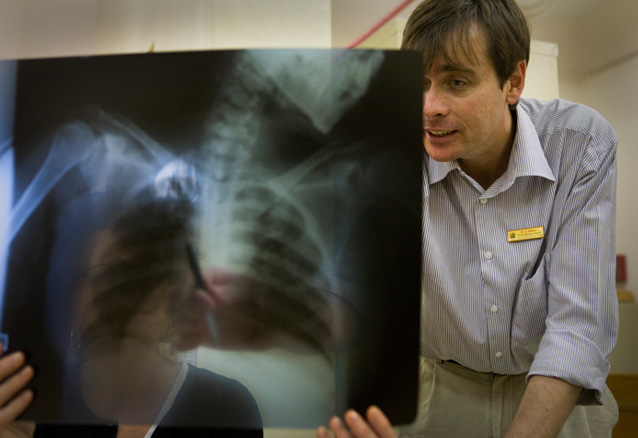
In addition to treating patients, physician Doug Wilson at state-run Edendale Hospital is working to develop a TB test for cases that cannot be diagnosed by X-ray and other means. The 900-bed hospital saw more than 10,000 patients in 2009, up from 3,000 patients in 2005. Of the patients admitted to the hospital, 50 percent are HIV-positive. Of those, half are also infected with TB.
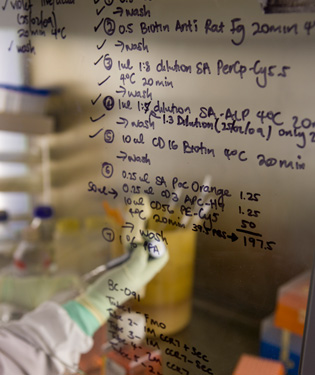

K-RITH will lend support to existing research programs in KwaZulu-Natal province. These programs include the development of a rapid diagnostic test for TB, the effort to identify whether certain people are more susceptible to TB or HIV infection, and the search for better treatments for HIV/TB co-infection.

A major goal of K-RITH is to train African scientists in cutting-edge lab techniques. As native Kenyan Thumbi NDung’u points out, it is vital that Africans be part of the process. NDung’u is a Harvard-trained researcher at the Nelson Mandela School of Medicine in Durban.

K-RITH was officially launched on March 19, 2009, with a press conference held in Washington, D.C., and televised simultaneously at the University of KwaZulu-Natal. Salim S. Abdool Karim, pro vice-chancellor for research at the University of KwaZulu-Natal, talks about his efforts to find out whether TB recurrence in HIV patients is caused by a new infection or an old infection that has been reactivated. Abdool Karim and other scientists gave presentations and took questions from the audience.

Journalists who attended the press conference were given opportunities to interview the participants, including then HHMI President Thomas Cech, who helped spearhead development of the international research center.

At the press conference, His Excellency Welile Nhlapo, the South African Ambassador to the United States, and Professor Malegapuru William Makgoba, vice-chancellor of the University of KwaZulu-Natal, joined with Cech in sealing the partnership with a handshake.